Vagus Nerve
There is a single nerve running from your brainstem all the way to your gut that quietly controls your heart rate, your digestion, your immune response, and even how quickly you calm down after a stressful event. Most people have never heard of it, yet it may be the most important nerve in your entire body. What if the key to reducing <a href='/g/anxiety-management.html'>anxiety</a>, improving <a href='/g/sleep-quality.html'>sleep quality</a>, and strengthening your <a href='/g/immune-system.html'>immune system</a> was already inside you, waiting to be activated?
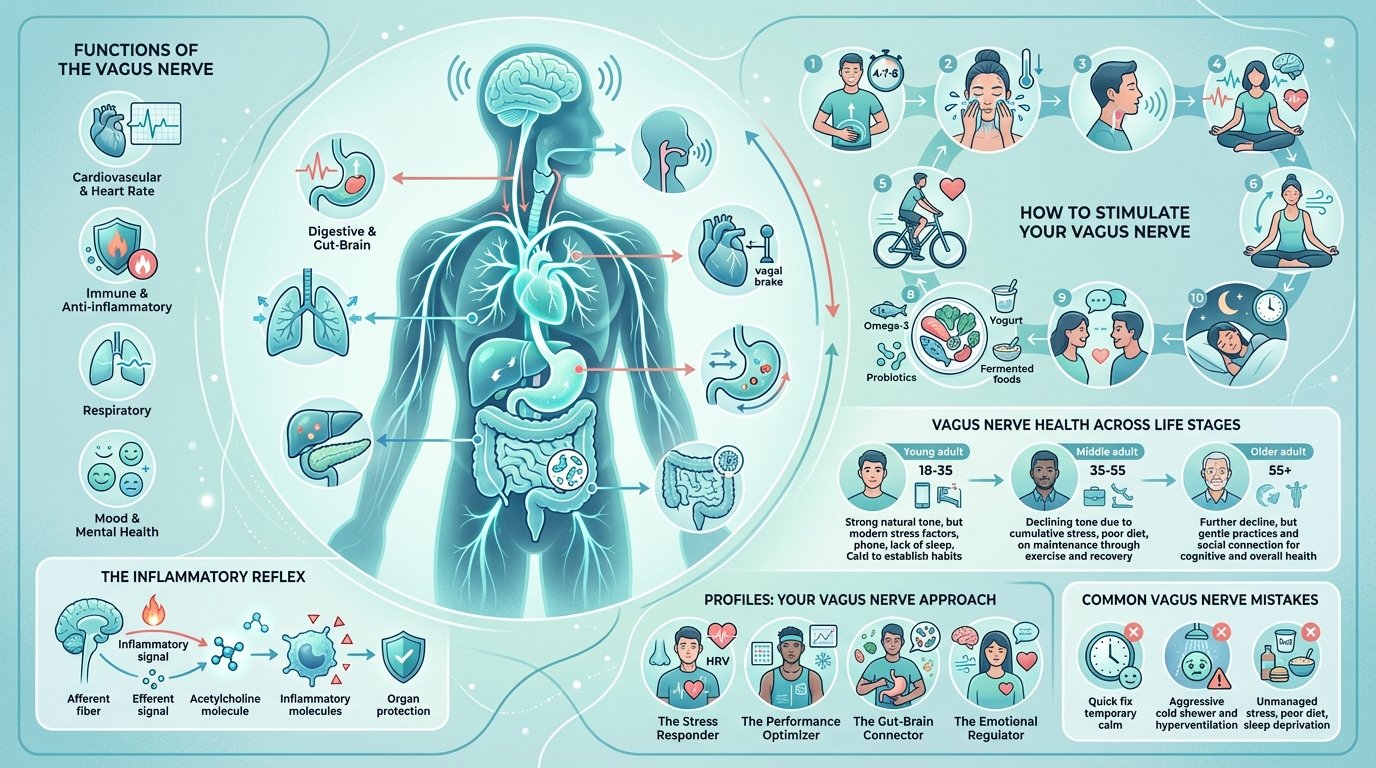
In this guide, you will learn exactly what the vagus nerve does, how it shapes your <a href='/g/mental-health.html'>mental health</a> and physical wellbeing, and the specific science-backed techniques you can use today to strengthen your vagal tone for lasting health benefits.
Whether you are dealing with chronic stress, digestive issues, or simply want to optimize your brain health, understanding the vagus nerve is a powerful first step toward a healthier, more resilient you.
What Is the Vagus Nerve?
The vagus nerve is the longest cranial nerve in the human body, stretching from the brainstem through the neck and chest all the way down to the abdomen. Its name comes from the Latin word vagus, meaning wandering, which perfectly describes its extensive path through nearly every major organ system. As the 10th cranial nerve (CN X), it serves as the primary communication highway between your brain and your gut, heart, lungs, and other vital organs. The vagus nerve contains approximately 80 percent sensory (afferent) fibers that carry information from the body to the brain, and 20 percent motor (efferent) fibers that send commands from the brain back to the body.
Not medical advice.
The vagus nerve is the main nerve of the parasympathetic nervous system, which is often called the rest-and-digest system. It controls involuntary body functions including heart rate, digestion, respiratory rate, and immune response. Your left and right vagal nerves contain about 75 percent of your parasympathetic nervous system's nerve fibers, making them essential for regulating your body's calm-and-recover functions. When the vagus nerve is functioning optimally, your body can efficiently shift between the fight-or-flight stress response and the relaxation response, which is critical for emotional regulation and overall holistic health.
Surprising Insight: Surprising Insight: The vagus nerve carries about 80 percent of all information flowing from your body to your brain, not the other way around. Your gut is constantly sending signals to your brain through the vagus nerve, which is why scientists now call the gut the second brain.
Vagus Nerve Pathway Through the Body
Shows how the vagus nerve connects the brainstem to major organ systems
🔍 Click to enlarge
Why the Vagus Nerve Matters in 2026
In a world where chronic stress has become the norm rather than the exception, the vagus nerve has emerged as a central focus of modern health science. Research published in recent years has revealed that poor vagal tone is linked to higher rates of anxiety disorders, depression, cardiovascular disease, and chronic inflammatory conditions. The U.S. Food and Drug Administration has approved vagus nerve stimulation (VNS) devices for treatment-resistant epilepsy and depression, and researchers are now investigating its potential for treating post-traumatic stress disorder, inflammatory bowel disease, and rheumatoid arthritis.
The concept of vagal tone has become increasingly important in understanding individual differences in stress resilience. High vagal tone is associated with better emotional resilience, faster recovery from stress, improved cognitive function, and stronger immune response. In 2010, researchers discovered a positive feedback loop between high vagal tone, positive emotions, and good physical health, meaning that improving your vagal tone creates an upward spiral of wellbeing. This discovery has made vagus nerve health a priority for anyone interested in biohacking and longevity.
Recent clinical trials have demonstrated that even simple, non-invasive techniques like deep breathing, cold exposure, and humming can measurably increase vagal tone within weeks. A randomized trial showed that just one week of daily transcutaneous auricular vagus nerve stimulation increased maximal oxygen uptake and reduced exercise-induced inflammation in healthy adults. This means that you do not need expensive devices or medical procedures to start improving your vagal function today.
The Science Behind the Vagus Nerve
The vagus nerve operates through a sophisticated bidirectional communication system known as the gut-brain axis. Through its afferent fibers, the vagus nerve continuously monitors the state of your internal organs and relays this information to the brainstem, which then coordinates appropriate responses. This monitoring includes detecting levels of inflammation, changes in gut microbiome composition, blood pressure fluctuations, and heart rhythm patterns. The efferent fibers of the vagus nerve then carry instructions back to the organs, adjusting heart rate, stimulating digestive enzymes, and modulating immune responses through what scientists call the cholinergic anti-inflammatory pathway.
One of the most important scientific discoveries about the vagus nerve is its role in controlling inflammation throughout the body. Neuroscientist Kevin Tracey identified what is now called the inflammatory reflex, where the vagus nerve acts as a brake on the immune system's inflammatory response. When the vagus nerve detects pro-inflammatory cytokines in the body, it triggers the release of acetylcholine, which inhibits the production of tumor necrosis factor (TNF) and other inflammatory molecules. This mechanism is central to disease prevention because chronic inflammation is now recognized as a driver of nearly all major chronic diseases, including heart disease, diabetes, Alzheimer's, and cancer. The vagus nerve essentially acts as your body's built-in anti-inflammatory system, and maintaining strong vagal tone helps keep this protective mechanism functioning at its best.
Vagus Nerve Inflammatory Reflex
How the vagus nerve detects and controls inflammation in the body
🔍 Click to enlarge
Understanding Vagal Tone
Vagal tone refers to the activity level of the vagus nerve and is typically measured through heart rate variability (HRV). Higher HRV generally indicates higher vagal tone, which means your parasympathetic nervous system is functioning well and your body can efficiently switch between states of alertness and relaxation. Think of vagal tone as a measure of how effectively your body can recover from stress. A person with high vagal tone will see their heart rate drop quickly after exercise or a stressful event, while someone with low vagal tone may remain in a heightened stress state for much longer.
Research has consistently linked high vagal tone to better health outcomes across nearly every system in the body. People with higher vagal tone tend to have lower blood pressure, better blood sugar regulation, improved digestive function, stronger immune responses, and reduced risk of cardiovascular events. On the psychological side, higher vagal tone is associated with greater emotional awareness, better coping strategies, increased empathy, and stronger social connections. The good news is that vagal tone is not fixed. Unlike many aspects of your biology, you can actively improve your vagal tone through consistent practice of specific techniques.
Measuring your vagal tone has become more accessible than ever with wearable technology. Many modern fitness trackers and smartwatches now measure HRV, giving you a daily snapshot of your vagal function. Tracking your HRV over time can help you understand how different lifestyle factors like sleep, exercise, stress, and nutrition affect your vagal tone. A typical healthy adult might have a resting HRV between 20 and 100 milliseconds, with higher values generally being better. Regular monitoring allows you to see which practices genuinely improve your vagal function and which may not be having the effect you expect.
Key Functions of the Vagus Nerve
Heart Rate and Cardiovascular Regulation
The vagus nerve is the primary regulator of your resting heart rate. It continuously releases acetylcholine to slow the heart, creating what is known as vagal brake. When you need to increase your heart rate during exercise or stress, the vagal brake is released. This delicate balance is essential for cardiovascular health. Impaired vagal control of the heart is associated with an increased risk of arrhythmias, hypertension, and heart failure. Research has shown that vagus nerve stimulation can improve heart rate variability and reduce the risk of dangerous heart rhythm disturbances, which is why heart health experts are increasingly focused on vagal function as a key health marker.
Digestive System and Gut-Brain Axis
The vagus nerve plays a critical role in digestion by stimulating the production of stomach acid, digestive enzymes, and bile. It also controls the rhythmic contractions (peristalsis) that move food through your gastrointestinal tract. When vagal function is impaired, you may experience symptoms like bloating, constipation, nausea, or gastroparesis (delayed stomach emptying). The gut-brain axis, largely mediated by the vagus nerve, also means that your gut health directly influences your mood and cognitive health. About 95 percent of your body's serotonin is produced in the gut, and the vagus nerve is the main pathway by which gut-produced neurotransmitters communicate with the brain.
Immune System Modulation
Through the cholinergic anti-inflammatory pathway, the vagus nerve acts as a critical regulator of immune function. It can detect inflammatory molecules in the bloodstream and respond by dampening excessive immune responses. This is crucial because while inflammation is necessary for fighting infections and healing injuries, chronic unchecked inflammation contributes to conditions like autoimmune diseases, metabolic syndrome, and neurodegenerative disorders. Studies have demonstrated that electrical vagus nerve stimulation can reduce inflammatory markers in patients with rheumatoid arthritis and Crohn's disease, opening new therapeutic avenues for disease prevention and management.
Mood Regulation and Mental Health
The vagus nerve has a profound impact on emotional wellness and mental health. It directly communicates with the limbic system, which governs emotions, and influences the production and regulation of key neurotransmitters including serotonin, GABA, and norepinephrine. The FDA-approved use of vagus nerve stimulation for treatment-resistant depression highlights its significance in mood regulation. Research suggests that people with anxiety disorders, PTSD, and depression often have reduced vagal tone, and interventions that increase vagal activity have been shown to improve symptoms. Practices like meditation, breathing exercises, and mindfulness may exert their beneficial mental health effects partly through vagus nerve activation.
| Body System | Vagus Nerve Function | Health Impact of Poor Vagal Tone |
|---|---|---|
| Cardiovascular | Regulates heart rate and blood pressure | Higher risk of arrhythmias and hypertension |
| Digestive | Controls stomach acid, enzymes, and peristalsis | Bloating, gastroparesis, IBS symptoms |
| Immune | Modulates inflammatory response via acetylcholine | Chronic inflammation and autoimmune risk |
| Respiratory | Regulates breathing rate and airway function | Breathing irregularities, asthma worsening |
| Neurological | Facilitates neurotransmitter production | Depression, anxiety, cognitive decline |
| Metabolic | Influences insulin secretion and glucose regulation | Insulin resistance and metabolic syndrome |
How to Stimulate Your Vagus Nerve: Step by Step
- Step 1: Practice slow diaphragmatic breathing: Inhale slowly for 4 seconds, allowing your belly to expand fully. Hold for 7 seconds, then exhale slowly through pursed lips for 8 seconds. This extended exhale directly stimulates the vagus nerve and activates the parasympathetic response. Practice this <a href='/g/4-7-8-breathing.html'>4-7-8 breathing pattern</a> for 4 cycles, twice daily.
- Step 2: Try cold water exposure: Splash cold water on your face or place a cold pack on the back of your neck for 30 seconds. Cold exposure activates the diving reflex, which stimulates the vagus nerve and slows your heart rate. Gradually work up to <a href='/g/biohacking.html'>cold showers</a> or cold water immersion for more profound vagal activation.
- Step 3: Hum, sing, or chant: The vagus nerve passes through the vocal cords and inner ear. Humming, singing loudly, chanting 'om,' or even gargling vigorously creates vibrations that mechanically stimulate the vagus nerve. Try humming for 5 minutes daily as part of your <a href='/g/morning-rituals.html'>morning routine</a>.
- Step 4: Practice meditation and mindfulness: Regular <a href='/g/meditation.html'>meditation practice</a> has been shown to increase vagal tone over time. Even 10 minutes of focused <a href='/g/mindfulness.html'>mindfulness</a> or loving-kindness meditation can produce measurable improvements in heart rate variability and vagal function.
- Step 5: Engage in regular aerobic exercise: Moderate-intensity <a href='/g/cardio-exercise.html'>cardio exercise</a> such as brisk walking, swimming, or cycling for 30 minutes most days has been shown to improve vagal tone. <a href='/g/exercise.html'>Exercise</a> trains the autonomic nervous system to become more flexible and responsive.
- Step 6: Try gentle yoga and stretching: <a href='/g/flexibility.html'>Flexibility</a> practices like yoga, particularly poses that involve bending, twisting, and inversions, can stimulate the vagus nerve. The combination of movement, breath control, and body awareness makes yoga one of the most comprehensive vagal toning practices available.
- Step 7: Massage the carotid sinus area: Gently massaging the right side of your neck where the carotid artery pulses can stimulate vagal fibers. Light circular massage of the neck and behind the ears for 2 to 3 minutes activates parasympathetic pathways. Always use gentle pressure and stop if you feel dizzy.
- Step 8: Eat a gut-healthy diet: Since the vagus nerve is the main communication link between your gut and brain, supporting your <a href='/g/gut-health.html'>gut microbiome</a> with fiber-rich foods, fermented foods, and probiotics can positively influence vagal signaling. Omega-3 fatty acids from fish have also been shown to stimulate vagus nerve activity.
- Step 9: Practice social connection: Positive social interactions and feelings of connection activate the vagus nerve through the social engagement system. Spending quality time with loved ones, making eye contact, and engaging in meaningful <a href='/g/communication.html'>conversation</a> all promote vagal activation and emotional <a href='/g/connection.html'>connection</a>.
- Step 10: Prioritize quality sleep: The vagus nerve is most active during <a href='/g/deep-sleep.html'>deep sleep</a> stages, which is when much of the body's repair and <a href='/g/healing-and-repair.html'>healing</a> takes place. Establishing consistent <a href='/g/evening-routines.html'>evening routines</a> and maintaining good <a href='/g/sleep-quality.html'>sleep hygiene</a> supports vagal recovery and helps reset your <a href='/g/circadian-rhythm.html'>circadian rhythm</a>.
Vagus Nerve Health Across Life Stages
Young Adulthood (18-35)
In young adulthood, vagal tone is typically at its highest natural level, but modern lifestyle factors can significantly degrade it. Chronic stress from career pressure, sleep deprivation from social obligations, and excessive screen time all suppress vagal function during this critical period. Young adults who establish strong vagus nerve health habits early, such as regular breathing practices, consistent exercise, and stress management techniques, build a foundation of resilience that pays dividends for decades. This is also the ideal time to develop a regular mindfulness practice, as the neural pathways strengthened during this period become more robust with time. Young adults dealing with anxiety or difficulty with emotional regulation often find that vagal toning exercises provide noticeable relief within just a few weeks of consistent practice.
Middle Adulthood (35-55)
During middle adulthood, vagal tone naturally begins to decline, making proactive maintenance increasingly important. This is the period when the consequences of chronic stress, poor diet, sedentary behavior, and inadequate recovery most visibly affect vagal function. Middle-aged adults who prioritize vagal health through regular cardiovascular exercise, meditation, and anti-inflammatory nutrition can maintain or even improve their vagal tone compared to younger adults who neglect these practices. This age group benefits particularly from HRV monitoring, as it provides objective feedback on how lifestyle choices impact vagal function. The risk of cardiovascular disease, metabolic syndrome, and burnout increases during this stage, making vagal health a critical component of comprehensive health management.
Later Adulthood (55+)
In later adulthood, vagal tone continues to decline naturally, and maintaining it becomes essential for preserving independence, cognitive function, and quality of life. Reduced vagal tone in older adults is associated with increased inflammation, slower recovery from illness, and higher risk of chronic disease. However, research shows that older adults respond well to vagal toning interventions. Gentle practices like deep breathing exercises, light yoga, tai chi, and social engagement can significantly improve vagal function in this population. The connection between vagal tone and brain health is especially relevant for older adults, as higher vagal tone is associated with better memory, attention, and reduced risk of cognitive decline. Maintaining strong social bonds and engaging in regular gentle movement are among the most effective strategies for supporting vagal health in later life.
Profiles: Your Vagus Nerve Approach
The Stress Responder
- Regular breathing exercises to activate parasympathetic recovery
- Consistent HRV tracking to identify stress patterns
- Daily micro-practices for nervous system regulation
Common pitfall: Waiting until burnout hits before addressing vagal health, then trying too many techniques at once and feeling overwhelmed.
Best move: Start with just two minutes of <a href='/g/box-breathing-techniques.html'>box breathing</a> each morning before checking your phone. Build consistency before adding complexity.
The Performance Optimizer
- Data-driven HRV monitoring for training and recovery
- Cold exposure protocols for vagal activation
- Strategic recovery practices between intense efforts
Common pitfall: Overtraining and chronic sympathetic dominance, which actually reduces vagal tone despite high fitness levels.
Best move: Use HRV as a guide for training intensity. On low HRV days, prioritize <a href='/g/recovery-optimization.html'>recovery</a> and gentle vagal stimulation over pushing harder.
The Gut-Brain Connector
- Gut microbiome support through diet and probiotics
- Mindful eating practices to enhance vagal digestion signals
- Stress reduction to prevent gut-brain axis disruption
Common pitfall: Focusing only on supplements and diet while ignoring the stress-driven nervous system imbalance that disrupts gut function.
Best move: Combine <a href='/g/gut-health.html'>gut-healthy nutrition</a> with daily vagal toning exercises. A healthy gut microbiome and strong vagal tone work together synergistically.
The Emotional Regulator
- Mindfulness and meditation for vagal activation
- Social connection practices for co-regulation
- Breathwork techniques for acute emotional regulation
Common pitfall: Using only cognitive strategies for emotional regulation while neglecting the body-based vagal pathways that are often more effective.
Best move: When emotions feel overwhelming, use <a href='/g/breathwork-for-emotional-healing.html'>breathwork</a> first to activate the vagus nerve and calm the nervous system before trying to think your way through the situation.
Common Vagus Nerve Mistakes
One of the most common mistakes people make is treating vagus nerve stimulation as a quick fix rather than a consistent practice. Many people try deep breathing or cold exposure once, feel temporarily better, and then abandon the practice when they do not see permanent changes overnight. Vagal toning is like building physical strength: it requires regular, consistent effort over weeks and months to produce lasting changes in your nervous system. Research suggests that meaningful improvements in vagal tone typically require at least four to six weeks of daily practice.
Another frequent error is overstimulating the vagus nerve through aggressive techniques without proper preparation. Jumping into extreme cold exposure, hyperventilation-style breathing patterns, or intense gargling sessions can actually trigger vagal syncope (fainting) in some individuals. The vagus nerve responds best to gentle, gradual stimulation. Start with mild cold water on your face before attempting full cold showers. Begin with simple diaphragmatic breathing before trying advanced breathwork protocols. If you feel dizzy, lightheaded, or nauseous during any vagal stimulation technique, stop immediately and consult with your healthcare provider.
A third mistake is ignoring the lifestyle factors that chronically suppress vagal tone. No amount of breathing exercises will compensate for chronic sleep deprivation, excessive alcohol consumption, a processed food diet, or unmanaged chronic stress. The most effective approach to vagus nerve health is comprehensive, addressing sleep quality, nutrition, physical activity, stress management, and social connection as an integrated system rather than relying on a single technique in isolation. Think of vagal health as a holistic wellness practice that touches every aspect of your daily life.
Vagus Nerve Stimulation Methods Compared
Comparing different vagal stimulation techniques by accessibility and evidence strength
🔍 Click to enlarge
Vagus Nerve and Breathing Techniques
Breathing is the most accessible and well-researched method for vagus nerve stimulation. The key principle is that slow breathing with an extended exhale activates the parasympathetic nervous system through the vagus nerve. During inhalation, your heart rate naturally speeds up slightly as the vagal brake is temporarily released. During exhalation, the vagal brake is reapplied and your heart rate slows. By making your exhale longer than your inhale, you spend more time in vagal activation, which gradually strengthens vagal tone over time. Research published in Frontiers in Human Neuroscience has shown that breathing at a rate of about six breaths per minute (a 5-second inhale followed by a 5-second exhale) produces the strongest vagal stimulation effects.
Several specific breathing techniques have strong evidence for vagal activation. The 4-7-8 technique (inhale for 4 counts, hold for 7, exhale for 8) is excellent for calming the nervous system before sleep. Box breathing (4 counts in, 4 counts hold, 4 counts out, 4 counts hold) is particularly effective for maintaining composure during stressful situations. Alternate nostril breathing balances the two branches of the autonomic nervous system. Coherence breathing, where you maintain equal inhale and exhale durations at about 5 seconds each, is considered the gold standard for sustained vagal toning and is used in many clinical research studies.
Vagus Nerve, Cold Exposure and Biohacking
Cold exposure is one of the most powerful acute vagus nerve stimulators available. When your face or body encounters cold water or air, it triggers the mammalian diving reflex, a survival mechanism that slows heart rate, constricts peripheral blood vessels, and redirects blood flow to vital organs. This reflex is mediated primarily by the vagus nerve. Research has shown that regular cold exposure can increase parasympathetic activity, reduce resting heart rate, and improve stress resilience over time. Many biohacking protocols now include cold exposure as a cornerstone practice specifically for its vagal toning benefits.
For beginners, the simplest entry point is splashing cold water on your face for 15 to 30 seconds. This targets the trigeminal nerve, which connects to the vagus nerve and triggers the diving reflex without the shock of full-body cold immersion. From there, you can progress to ending your shower with 30 seconds of cold water, gradually increasing duration and decreasing temperature over weeks. Advanced practitioners may benefit from cold plunge sessions lasting 2 to 5 minutes at temperatures between 50 and 59 degrees Fahrenheit. The key is consistency rather than extremity. A daily 30-second cold face splash will produce better vagal toning results over time than an occasional extreme cold plunge followed by weeks of avoidance.
Nutrition and Gut Health for Vagal Function
The gut-brain axis is one of the most important pathways of vagal communication, and your diet directly influences the signals your gut sends to your brain through the vagus nerve. A diverse, fiber-rich diet supports a healthy gut microbiome, which in turn produces short-chain fatty acids and neurotransmitters that activate vagal afferent fibers. Fermented foods like yogurt, kefir, sauerkraut, and kimchi contain beneficial bacteria that have been shown to positively modulate vagal signaling. Studies have found that specific probiotic strains, particularly Lactobacillus rhamnosus, can reduce anxiety-like behavior through the vagus nerve, an effect that disappears when the vagus nerve is cut.
Omega-3 fatty acids, found abundantly in fatty fish like salmon, mackerel, and sardines, have been shown to increase heart rate variability and improve vagal tone. Anti-inflammatory foods rich in polyphenols, such as berries, green tea, turmeric, and dark chocolate, support vagal function by reducing systemic inflammation. Conversely, highly processed foods, excessive sugar, and artificial additives can disrupt the gut microbiome and impair vagal signaling. A Mediterranean-style diet, rich in vegetables, fruits, whole grains, fish, and olive oil, closely aligns with what the research suggests is optimal for vagal health and overall wellbeing. Supplements like omega-3 fish oil, zinc, and B vitamins may also support vagal function when dietary intake is insufficient.
| Food or Nutrient | Vagal Benefit | Recommended Sources |
|---|---|---|
| Omega-3 fatty acids | Increases HRV and vagal tone | Salmon, mackerel, sardines, walnuts |
| Probiotics | Improves gut-brain vagal signaling | Yogurt, kefir, sauerkraut, kimchi |
| Dietary fiber | Feeds beneficial gut bacteria for SCFA production | Oats, beans, lentils, vegetables |
| Polyphenols | Reduces inflammation that impairs vagal function | Berries, green tea, dark chocolate, turmeric |
| Zinc | Supports neurotransmitter synthesis via vagal pathways | Oysters, beef, pumpkin seeds, chickpeas |
Science and Studies
The scientific evidence supporting vagus nerve health practices has grown substantially in recent years. Here is a summary of key research findings that inform the techniques and recommendations in this guide. Each of these studies has been published in peer-reviewed journals and contributes to our understanding of how the vagus nerve influences health, emotional health, and cognitive performance.
- Breit et al. (2018), Frontiers in Psychiatry: Comprehensive review confirming the vagus nerve as modulator of the brain-gut axis in psychiatric and inflammatory disorders, establishing the role of vagal tone in depression and anxiety treatment.
- Tracey (2002), Nature: Landmark paper identifying the inflammatory reflex and the cholinergic anti-inflammatory pathway, demonstrating how the vagus nerve controls systemic inflammation through acetylcholine release.
- Kok & Fredrickson (2010), Psychological Science: Discovered the positive feedback loop between vagal tone, positive emotions, and physical health, showing that vagal tone can be improved through loving-kindness meditation.
- Gerritsen & Band (2018), Frontiers in Human Neuroscience: Demonstrated that slow controlled breathing at approximately 6 breaths per minute optimally stimulates vagal afferent pathways and improves heart rate variability.
- Bonaz et al. (2018), Frontiers in Neuroscience: Reviewed clinical applications of vagus nerve stimulation for inflammatory bowel disease, establishing the therapeutic potential of targeting the vagal anti-inflammatory pathway.
Your First Micro Habit
Start Small Today
Today's action: Every morning before getting out of bed, take 5 slow breaths with a 4-second inhale and 8-second exhale. This 60-second practice directly stimulates your vagus nerve and sets a calm parasympathetic tone for the entire day.
Extended exhale breathing activates the vagal brake on your heart rate, triggering the parasympathetic relaxation response. Doing it first thing in the morning trains your nervous system to default to calm rather than reactive stress. Research shows that even brief breathing exercises can measurably increase heart rate variability within minutes.
Track your micro habits and get personalized AI coaching with our app.
Quick Assessment
When faced with a stressful situation, how does your body typically respond?
Your stress recovery speed reflects your vagal tone. Faster recovery suggests stronger parasympathetic function, while prolonged stress responses may indicate an opportunity to strengthen your vagus nerve through targeted practices.
How would you describe your current digestive health?
Digestive function is closely tied to vagal activity. The vagus nerve controls stomach acid production, enzyme release, and gut motility. Improving vagal tone often leads to noticeable improvements in digestive comfort.
Which approach to wellness resonates most with you?
Your preferred approach suggests the best starting point for your vagus nerve practice. All methods are effective, and the best one is the one you will actually do consistently. Over time, combining multiple approaches produces the strongest results.
Take our full assessment to get personalized recommendations for your vagus nerve health journey.
Discover Your Wellness Style →Next Steps
You now understand the critical role the vagus nerve plays in connecting your brain to your body's most important systems. From heart health and digestive function to immune regulation and emotional balance, the vagus nerve is truly the master regulator of your body's rest, repair, and recovery systems. The techniques outlined in this guide, from breathing exercises to cold exposure and meditation, are all within your reach starting today. Begin with the micro habit of five slow breaths each morning and gradually add more practices as they become part of your natural daily routine.
To deepen your understanding and build a truly comprehensive approach to nervous system health, explore our related guides on brain optimization, stress management, emotional resilience, and holistic health. Each of these topics connects directly to vagal function and together they form the foundation of a life built on genuine body wellness and lasting health. Track your progress, stay consistent, and remember that every breath you take with intention is strengthening the most important nerve in your body.
Get personalized guidance with AI coaching.
Start Your Journey →Research Sources
This article is based on peer-reviewed research and authoritative sources. Below are the key references we consulted:
Related Glossary Articles
Frequently Asked Questions
What happens when the vagus nerve is not functioning properly?
When vagal function is impaired, also called low vagal tone, you may experience a wide range of symptoms including chronic anxiety, difficulty calming down after stress, digestive problems like bloating and gastroparesis, elevated resting heart rate, chronic inflammation, weakened immune response, and difficulty with emotional regulation. Low vagal tone is associated with higher risk of cardiovascular disease, autoimmune conditions, depression, and metabolic disorders.
How long does it take to improve vagal tone?
Most research suggests that consistent daily practice of vagal stimulation techniques like slow breathing, meditation, or cold exposure can produce measurable improvements in heart rate variability within 4 to 8 weeks. Some people notice subjective improvements in stress response and emotional regulation within the first 1 to 2 weeks. The key is daily consistency rather than occasional intense sessions. Like building physical fitness, vagal toning is a gradual process that continues to improve with sustained practice.
Can you damage the vagus nerve through stimulation exercises?
Gentle, non-invasive vagal stimulation techniques like breathing exercises, humming, and moderate cold exposure are generally very safe for healthy individuals. However, overly aggressive techniques can cause vasovagal syncope (fainting) in some people. If you experience dizziness, lightheadedness, or nausea during any vagal exercise, stop immediately. People with heart conditions, low blood pressure, epilepsy, or who are pregnant should consult their healthcare provider before beginning vagal stimulation practices.
What is the difference between vagus nerve stimulation devices and natural techniques?
Medical vagus nerve stimulation (VNS) devices deliver controlled electrical impulses directly to the vagus nerve and are FDA-approved for treatment-resistant epilepsy and depression. They require surgical implantation or medical-grade transcutaneous devices. Natural techniques like breathing exercises, cold exposure, singing, and meditation stimulate the vagus nerve indirectly through sensory pathways. While less precise than devices, natural techniques are free, accessible, and backed by significant research showing they can meaningfully improve vagal tone over time.
How can I measure my vagal tone at home?
The most practical way to measure vagal tone at home is through heart rate variability (HRV) monitoring. Many modern smartwatches and fitness trackers measure HRV, and dedicated HRV apps can work with external chest strap monitors for more accurate readings. Higher HRV generally indicates better vagal tone. Track your HRV at the same time each day, ideally first thing in the morning, to establish your baseline and monitor changes over time. Look for trends over weeks rather than focusing on daily fluctuations.
Does the vagus nerve affect mental health and mood?
Yes, significantly. The vagus nerve directly influences the production and regulation of key neurotransmitters including serotonin, GABA, and norepinephrine, all of which play central roles in mood regulation. About 95 percent of serotonin is produced in the gut and communicated to the brain via the vagus nerve. The FDA has approved vagus nerve stimulation for treatment-resistant depression, and research shows that people with anxiety disorders and PTSD often have reduced vagal tone. Improving vagal function through breathing, meditation, and lifestyle practices can meaningfully support mental health.
Take the Next Step
Ready to improve your wellbeing? Take our free assessment to get personalized recommendations based on your unique situation.
- Discover your strengths and gaps
- Get personalized quick wins
- Track your progress over time
- Evidence-based strategies