Trauma Bonding
You know something is wrong. The relationship leaves you drained, confused, and questioning your own reality. Yet every time you try to walk away, an invisible force pulls you back. You find yourself defending the very person who hurts you, replaying their rare moments of kindness like a highlight reel that erases weeks of pain. If this cycle sounds familiar, you may be experiencing <a href="/g/trauma-bonding.html">trauma bonding</a>, one of the most powerful and misunderstood psychological dynamics in human relationships.
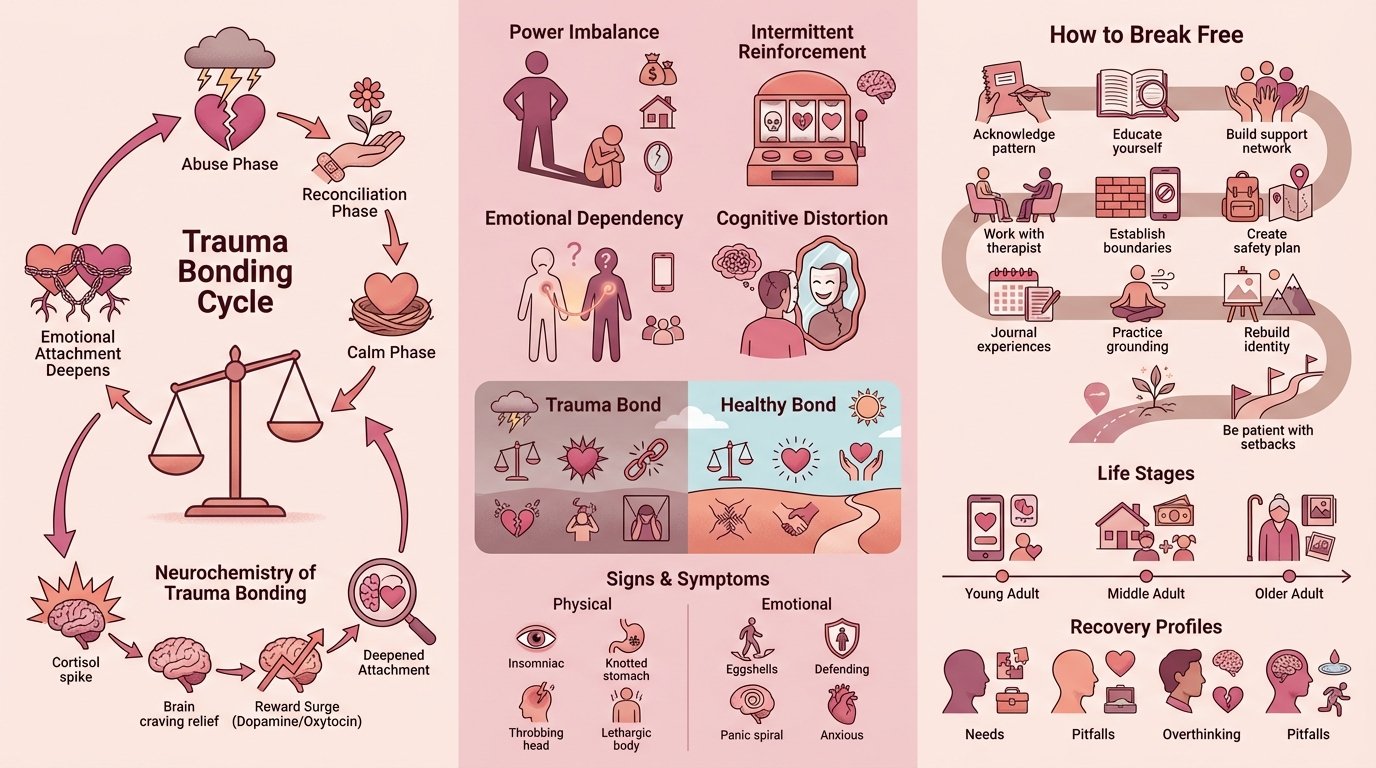
In this guide, you will learn exactly how trauma bonds form, why your brain chemistry works against you, and the concrete steps that therapists and researchers recommend for breaking free. Understanding the mechanics behind this pattern is the first step toward reclaiming your <a href="/g/emotional-health.html">emotional health</a> and building the <a href="/g/healthy-relationship-habits.html">healthy relationship habits</a> you deserve.
Whether you are currently in a difficult relationship, supporting someone who is, or simply want to understand this phenomenon better, this article draws on decades of clinical research to give you actionable knowledge. By the end, you will have a clear roadmap for emotional healing and a deeper understanding of your own attachment styles.
What Is Trauma Bonding?
Trauma bonding is a strong emotional attachment that forms between a person and their abuser through a cyclical pattern of abuse and intermittent positive reinforcement. First described by Patrick Carnes, Ph.D. in 1997, trauma bonding occurs when repeated cycles of mistreatment are followed by periods of affection, creating a powerful psychological dependency. Carnes defined it as an adaptive, dysfunctional attachment occurring in the presence of danger, shame, or exploitation in order to survive. The term captures how the victim's emotional connection to their abuser becomes neurologically reinforced over time.
Not medical advice.
Trauma bonds can form in many contexts beyond romantic relationships. They occur in parent-child relationships, cults, hostage situations, workplace bullying, sex trafficking, and military hazing. The common thread is always a power imbalance combined with intermittent reinforcement, where unpredictable alternation between cruelty and kindness creates confusion and dependency. Understanding that trauma bonding is a normal neurobiological response to abnormal circumstances is essential. It does not reflect weakness or a character flaw. It reflects the brain doing exactly what it evolved to do: attach to a source of both danger and perceived safety. This understanding is central to building genuine self-compassion during recovery.
Surprising Insight: Surprising Insight: Research shows that intermittent reinforcement, the pattern at the heart of trauma bonding, creates stronger behavioral attachments than consistent positive reinforcement. This is the same mechanism that makes gambling addictive, and it explains why trauma-bonded individuals often feel more intensely attached than people in healthy, stable relationships.
The Trauma Bonding Cycle
How the cycle of abuse and reconciliation creates and reinforces a trauma bond
🔍 Click to enlarge
Why Trauma Bonding Matters in 2026
Awareness of trauma bonding has grown significantly in recent years, yet misconceptions remain widespread. Many people still blame victims for staying in abusive relationships, not understanding the neurochemical processes that make leaving feel physically and emotionally impossible. In a world where mental health awareness is finally being taken seriously, understanding trauma bonding is crucial for supporting survivors and preventing ongoing harm. Greater public literacy about this topic can save lives.
Digital technology has created new avenues for trauma bonding to develop and intensify. Social media, constant messaging, and location tracking give abusers unprecedented tools for monitoring and controlling their partners. The cycle of public praise followed by private cruelty can be amplified through online platforms, making it harder for victims to recognize the pattern. Building strong emotional boundaries in digital spaces is more important than ever for protecting your emotional wellbeing.
Research into trauma bonding also has implications far beyond individual relationships. Understanding how these bonds form helps us recognize coercive dynamics in workplaces, political movements, and institutions. When we learn to identify the hallmarks of intermittent reinforcement and power imbalance, we develop stronger emotional awareness that protects us across all areas of life. This knowledge supports broader resilience at both individual and societal levels.
The Science Behind Trauma Bonding
The neuroscience of trauma bonding involves three key chemicals working together to create addiction-like dependency. Cortisol, the stress hormone, floods the brain during abusive episodes, keeping the victim in a state of heightened alertness. Dopamine surges during the reconciliation phase when the abuser shows kindness, creating an intense sense of relief and pleasure that the brain codes as a reward. Oxytocin, often called the bonding hormone, is released during moments of perceived closeness, deepening the attachment patterns even when the relationship is harmful. This biochemical cocktail creates a powerful feedback loop where the abuser becomes both the source of fear and the perceived source of safety.
Intermittent reinforcement is the psychological mechanism that makes trauma bonds so difficult to break. When rewards are delivered on an unpredictable schedule, the brain becomes hypervigilant and fixated on detecting the next reward. This is the same principle that drives gambling addiction: the uncertainty of when the next positive moment will arrive makes those moments exponentially more powerful than predictable kindness. Research by psychologist B.F. Skinner demonstrated that intermittent reinforcement schedules produce the strongest and most extinction-resistant behaviors. In the context of an abusive relationship, this means the victim becomes neurologically wired to crave and seek out the abuser's approval, even at tremendous personal cost to their self-worth and emotional resilience.
Trauma bonding also involves cognitive distortions that develop as the brain attempts to make sense of contradictory experiences. Cognitive dissonance, the mental discomfort of holding two conflicting beliefs simultaneously, pushes the victim to rationalize the abuse. The brain resolves this tension by minimizing the negative experiences and amplifying the positive ones. Over time, this creates a distorted reality where the victim may genuinely believe the relationship is loving despite overwhelming evidence to the contrary. Working with a professional to rebuild accurate cognitive function and perception is a critical part of recovery.
The concept of learned helplessness further explains why trauma-bonded individuals struggle to leave. Research by Martin Seligman showed that when people are repeatedly exposed to uncontrollable negative situations, they eventually stop trying to escape, even when escape becomes possible. In trauma bonding, the unpredictable nature of the abuse erodes the victim's sense of agency, making them feel that nothing they do can change their situation. Rebuilding a sense of personal growth and confidence building is essential to counteracting this learned helplessness.
Neurochemistry of Trauma Bonding
How cortisol, dopamine, and oxytocin interact to reinforce the trauma bond
🔍 Click to enlarge
Key Components of Trauma Bonding
Power Imbalance
A significant power imbalance is the foundation of every trauma bond. This imbalance can be financial, emotional, physical, or social. The abuser maintains control by keeping the victim dependent, whether through isolating them from friends and family, controlling finances, or undermining their self-esteem. Recognizing where the power imbalance exists is a critical first step in understanding the dynamic. In healthy relationships, power is shared and negotiated. In trauma-bonded relationships, one person holds disproportionate influence over the other's daily experience, decision-making, and sense of self.
Intermittent Reinforcement
The unpredictable alternation between cruelty and kindness is what makes trauma bonds uniquely powerful. If the abuse were constant, the victim would have a clearer picture of the relationship and would be more likely to leave. It is the moments of genuine-seeming warmth, affection, and apology that create confusion. The abuser may buy gifts, express deep love, or make promises of change after an abusive episode. These moments of positive reinforcement are neurologically coded as rewards by the brain's dopamine system, creating a pattern similar to addiction. Understanding this mechanism is key to developing effective coping strategies for breaking free.
Emotional Dependency
Over time, the trauma-bonded person becomes emotionally dependent on the abuser for their sense of identity, worth, and even basic emotional regulation. The victim may feel unable to function without the abuser's approval or presence. This dependency is reinforced by isolation, as the abuser often works to cut the victim off from supportive friendships, family dynamics, and professional networks. Rebuilding independent emotional regulation skills and external support systems is essential for recovery.
Cognitive Distortion
Trauma bonding warps perception in measurable ways. Victims commonly engage in minimization, telling themselves the abuse was not that bad, or rationalization, finding reasons to justify the abuser's behavior. They may develop Stockholm Syndrome-like responses, defending their abuser to others and feeling protective of the relationship. These cognitive distortions are not signs of poor judgment; they are predictable neurological responses to chronic stress and intermittent reinforcement. Rebuilding accurate perception through mindfulness, journaling, and therapeutic support helps restore clarity and supports long-term behavioral change.
| Dimension | Trauma Bond | Healthy Bond |
|---|---|---|
| Power dynamic | One person controls; the other complies | Shared power and mutual respect |
| Emotional pattern | Extreme highs and lows; walking on eggshells | Consistent warmth with manageable disagreements |
| After conflict | Love bombing, excessive apologies, empty promises | Genuine accountability and changed behavior |
| Self-worth effect | Erodes confidence; you question your own reality | Builds confidence; you feel seen and valued |
| Leaving feels like | Withdrawal, panic, physical pain | Sadness but also relief and clarity |
Recognizing the Signs of Trauma Bonding
Recognizing trauma bonding can be challenging because the bond itself distorts your ability to see the relationship clearly. However, there are consistent warning signs that psychologists and counselors have identified. You may be in a trauma bond if you constantly make excuses for your partner's behavior, feel unable to leave despite knowing the relationship is harmful, experience intense anxiety at the thought of separation, or find yourself returning after every attempt to leave. Other signs include feeling responsible for the abuser's emotions, defending them to concerned friends and family, and believing that their moments of kindness represent their true self while the abuse is an aberration.
Physical symptoms often accompany trauma bonding. Chronic stress from the cycle of abuse can manifest as insomnia, digestive problems, headaches, and fatigue. Your body may react to the abuser's presence with a rush of adrenaline that you mistake for love or excitement. Paying attention to these physical signals and developing stronger emotional coping skills can help you recognize what your body already knows, even when your mind has not caught up. Integrating stress management practices into your daily life can provide the clarity needed to see the pattern.
It is also important to understand what trauma bonding is not. Genuine love and commitment in a healthy relationship can sometimes involve working through difficult periods, and this is not the same as trauma bonding. The distinction lies in the pattern: trauma bonding involves a consistent cycle of abuse followed by reconciliation, a persistent power imbalance, and a gradual erosion of the victim's autonomy and self-worth. In healthy relationships, both partners feel safe to express their needs, set boundaries, and maintain their individual identities.
How to Break Free from Trauma Bonding
- Step 1: Acknowledge the pattern. Write down specific instances of the abuse-reconciliation cycle. Seeing it on paper makes the pattern harder to deny. This first step requires honest <a href="/g/emotional-awareness.html">emotional awareness</a> and may feel overwhelming, but it is essential.
- Step 2: Educate yourself. Read about trauma bonding from credible psychology sources. Understanding the neurochemistry behind your attachment removes shame and replaces it with knowledge. Knowledge is the foundation of <a href="/g/personal-growth.html">personal growth</a>.
- Step 3: Build your support network. Reach out to trusted friends, <a href="/g/family-dynamics.html">family</a>, a therapist, or a domestic violence hotline. Isolation keeps the bond strong; <a href="/g/connection.html">connection</a> weakens it.
- Step 4: Work with a trauma-informed therapist. Professional guidance is invaluable for processing the complex emotions involved in breaking a trauma bond. Therapists trained in EMDR, somatic experiencing, or cognitive behavioral therapy can provide targeted <a href="/g/help-seeking.html">help</a>.
- Step 5: Establish no-contact or low-contact boundaries. Reducing or eliminating contact with the abuser disrupts the reinforcement cycle. This is often the hardest step but also the most effective for breaking the neurochemical loop. Strong <a href="/g/emotional-boundaries.html">emotional boundaries</a> are your greatest tool.
- Step 6: Create a safety plan. If leaving involves physical risk, work with a professional to develop a detailed exit strategy. This may include securing important documents, identifying a safe place to stay, and having an emergency contact.
- Step 7: Journal your experiences daily. Writing helps counteract the cognitive distortions that trauma bonding creates. Record both the abusive incidents and the good moments, then review them over time to see the pattern clearly. This builds <a href="/g/emotional-intelligence.html">emotional intelligence</a>.
- Step 8: Practice grounding techniques. When you feel the pull to return, use <a href="/g/breathing-techniques.html">breathing techniques</a>, body scans, or <a href="/g/meditation.html">meditation</a> to regulate your nervous system. The urge to return often comes from a cortisol-driven stress response, not genuine desire.
- Step 9: Rebuild your identity. Reconnect with hobbies, goals, and relationships that the abusive dynamic pushed aside. Rediscovering who you are outside of the bond strengthens your <a href="/g/self-esteem.html">self-esteem</a> and <a href="/g/self-improvement.html">self-improvement</a> journey.
- Step 10: Be patient with setbacks. Breaking a trauma bond is not linear. Relapses are common and do not mean failure. Each attempt to break free strengthens your <a href="/g/resilience.html">resilience</a>, even if it does not succeed immediately. Celebrate every step forward.
Trauma Bonding Across Life Stages
Young Adulthood (18-35)
Young adults are particularly vulnerable to trauma bonding because they are still forming their relational templates. First romantic relationships carry enormous weight, and early experiences of intermittent reinforcement can become normalized, making it difficult to recognize unhealthy patterns later. College students and young professionals who lack strong communication skills or experience with boundary setting may mistake intensity for intimacy. Social media and dating apps can accelerate the bonding process and make it harder to disengage. Building awareness of attachment styles early in adulthood provides a protective framework.
Middle Adulthood (35-55)
In middle adulthood, trauma bonds often become entangled with practical dependencies such as shared finances, children, and property. The stakes of leaving feel higher, and the abuser may use these shared responsibilities as leverage. Long-term trauma bonds in this life stage are often deeply embedded, with the victim having adapted their entire identity around the relationship. However, middle adulthood also brings accumulated wisdom and often stronger external support systems. People at this stage who recognize the pattern may find that their life experience gives them greater capacity for psychological flexibility and conflict resolution when navigating the exit process.
Later Adulthood (55+)
Older adults in trauma-bonded relationships face unique challenges including health dependencies, fixed incomes, and decades of ingrained patterns. They may have spent a lifetime rationalizing the abuse and may feel it is too late to change. However, research shows that it is never too late to break a trauma bond and experience emotional recovery. Support groups specifically designed for older adults, elder abuse hotlines, and community resources can provide the belonging and practical assistance needed. Building new sources of connection and meaning outside the relationship is possible at any age.
Profiles: Your Trauma Bonding Recovery Approach
The Analyzer
- Detailed information about the neuroscience of trauma bonding
- Data-driven evidence that what they are experiencing is real
- Structured frameworks for understanding the cycle
Common pitfall: Using intellectual understanding as a substitute for emotional processing, leading to overthinking without action
Best move: Pair your research with body-based practices like <a href="/g/breathing-techniques.html">breathing techniques</a> or somatic therapy to connect head knowledge with felt experience
The Caretaker
- Permission to prioritize their own needs without guilt
- Validation that leaving is not abandonment
- Support from people who model healthy <a href="/g/empathy.html">empathy</a> without enabling
Common pitfall: Staying in the bond because they feel responsible for the abuser's wellbeing or believe they can fix the person
Best move: Redirect your natural caregiving energy toward <a href="/g/self-compassion.html">self-compassion</a> and building a support circle that cares for you in return
The Action Taker
- A concrete, step-by-step exit plan
- Practical resources like financial planning and housing options
- Clear milestones to track progress
Common pitfall: Leaving abruptly without emotional processing, which can lead to returning when the withdrawal hits
Best move: Combine your action-oriented approach with ongoing therapy and <a href="/g/emotional-regulation.html">emotional regulation</a> practice to address the underlying attachment patterns
The Reflector
- Time and space for emotional processing through journaling or creative expression
- Gentle, non-judgmental validation of their experience
- A gradual approach that respects their pace
Common pitfall: Getting stuck in processing mode and using reflection as a way to avoid making difficult changes
Best move: Set gentle but firm timelines for action steps, and use your reflective nature to build a powerful <a href="/g/mindfulness.html">mindfulness</a> practice that supports long-term healing
Common Trauma Bonding Mistakes
One of the most common mistakes is believing that love alone can fix the situation. Many trauma-bonded individuals hold onto the hope that if they love harder, behave better, or find the right words, the abuser will change. This belief is reinforced by the reconciliation phases of the cycle when the abuser appears genuinely remorseful. However, genuine change in abusive patterns requires the abuser to take full responsibility and engage in sustained professional treatment. Waiting for this change while remaining in the bond only deepens the emotional damage and delays your own healing and growth.
Another mistake is isolating yourself during recovery. Breaking a trauma bond triggers genuine withdrawal symptoms similar to those experienced in substance addiction. During this period, you need more support, not less. Trying to recover alone makes you significantly more vulnerable to returning to the abuser. Building a strong network of friendships, joining a support group, and maintaining regular contact with a therapist provides the scaffolding your brain needs while it rewires itself. Do not underestimate the power of community and connection in the healing process.
A third mistake is rushing into a new relationship before processing the trauma bond. The brain patterns that created vulnerability to the original bond are still active, and without therapeutic work on your attachment styles and emotional boundaries, you risk recreating similar dynamics with a new partner. Taking time for genuine emotional recovery, building strong self-esteem, and developing healthy communication skills before entering a new relationship creates the foundation for healthier couple dynamics in the future.
Recovery Journey from Trauma Bonding
The stages of recovery from a trauma bond and key actions at each stage
🔍 Click to enlarge
Trauma Bonding and Related Concepts
Trauma bonding is closely related to Stockholm Syndrome, though the two are distinct. Stockholm Syndrome specifically describes an acute response to captivity where hostages develop positive feelings toward their captors as a survival strategy, typically over days or weeks. Trauma bonding develops gradually within ongoing relationships and involves a more complex interplay of attachment patterns, neurochemistry, and intermittent reinforcement. While Stockholm Syndrome victims are clearly held against their will, trauma-bonded individuals initially chose to participate in the relationship, which adds layers of self-blame and confusion.
Codependency and trauma bonding frequently overlap but are not identical. Codependency is a broader pattern of excessive emotional reliance on another person, often rooted in childhood experiences. A person can be codependent without being trauma-bonded, and vice versa. However, codependent tendencies can make someone more vulnerable to trauma bonding because they already have a template for deriving their sense of worth from another person's approval. Addressing both patterns often involves similar therapeutic approaches, including building assertiveness, strengthening self-worth, and developing independent emotional regulation.
Understanding the seven stages of trauma bonding, as described in clinical literature, provides a useful framework. These stages typically progress from love bombing, through trust and dependency, to criticism, gaslighting, resignation, loss of self, and finally addiction to the cycle. Recognizing which stage you are in can help you and your therapist develop targeted interventions. Each stage involves specific coping mechanisms that, while protective in the short term, ultimately keep the bond intact. Replacing these mechanisms with healthier alternatives is central to breakup recovery.
Building Healthy Relationships After Trauma Bonding
Recovery from a trauma bond is not just about leaving the abusive relationship; it is about fundamentally reshaping how you relate to others and yourself. This process involves relearning what healthy love looks and feels like, which can be disorienting at first. Healthy relationships may initially feel boring or lacking in intensity compared to the emotional rollercoaster of a trauma bond. This is normal. Your nervous system needs time to recalibrate and learn that trust, consistency, and calm presence are what genuine love feels like.
Developing a secure attachment style after trauma bonding requires deliberate practice. This means learning to tolerate vulnerability without catastrophizing, communicating needs directly instead of through hints or withdrawal, and allowing yourself to be seen fully by another person. Working with a therapist who specializes in attachment styles can accelerate this process. Building strong active listening skills and practicing conflict resolution in low-stakes situations helps develop the relational muscles that were atrophied during the trauma bond.
Self-compassion is perhaps the most important ingredient in post-trauma-bond recovery. Many survivors carry deep shame about having been in the bond, and this shame can become its own barrier to healing. Understanding that trauma bonding is a predictable neurobiological response, not a personal failing, is the first step toward self-compassion. Practices like forgiveness of yourself, gratitude practice, and acceptance of your journey create the emotional foundation for healthier future relationships.
Science and Studies
Decades of clinical research support our understanding of trauma bonding as a predictable neurobiological phenomenon rather than a character weakness. The following studies and frameworks have been particularly influential in shaping how therapists and researchers approach this topic. These findings underscore the importance of trauma-informed care and validate the experiences of survivors who struggle to leave abusive situations despite knowing they should.
- Patrick Carnes, Ph.D. (1997) - Coined the term 'trauma bonding' and described it as an adaptive, dysfunctional attachment in the presence of danger, shame, or exploitation.
- Dutton & Painter (1981, 1993) - Developed the theory of traumatic bonding based on power imbalance and intermittent reinforcement in abusive relationships.
- B.F. Skinner - Variable-ratio reinforcement research demonstrating that unpredictable reward schedules create the strongest and most extinction-resistant behavioral patterns.
- Martin Seligman - Learned helplessness research showing how repeated exposure to uncontrollable negative situations leads to passive acceptance even when escape is possible.
- van der Kolk, Bessel (2014) - 'The Body Keeps the Score' documented how trauma reshapes brain structure and function, including the neurobiological basis of trauma bonds.
Your First Micro Habit
Start Small Today
Today's action: Each evening, write one sentence about how you felt in your relationship today. Simply note: 'Today I felt _____ because _____.'' This takes less than sixty seconds and begins building the emotional awareness pattern that disrupts cognitive distortion.
Consistent micro-journaling creates a factual record that counteracts the memory distortion inherent in trauma bonding. Over time, patterns become visible that are impossible to see in the moment, supporting clearer perception and stronger emotional regulation.
Track your micro habits and get personalized AI coaching with our app.
Quick Assessment
When your partner hurts you and then shows unusual kindness afterward, how do you typically respond?
Your response reveals where you are in the awareness spectrum. Recognizing the cycle is the foundation; acting on that recognition requires building stronger coping strategies and support systems over time.
How do you feel when you imagine your life without this relationship?
Fear of separation is one of the strongest indicators of trauma bonding. The intensity of this fear often correlates with the strength of the bond and can guide your therapist in tailoring your recovery approach.
When friends or family express concern about your relationship, what is your first reaction?
How you respond to outside perspective reveals the degree of cognitive distortion present in the bond. Defensiveness is a hallmark of deep trauma bonding, while openness to feedback indicates growing emotional awareness.
Take our full assessment to get personalized recommendations for emotional health and relationship wellness.
Discover Your Wellbeing Profile →Next Steps
If you recognize trauma bonding patterns in your life, the most powerful thing you can do right now is acknowledge what you are experiencing without judgment. Start with the micro-journaling habit described above. Reach out to at least one trusted person and share what you have learned from this article. Explore our related guides on emotional healing, boundary setting, breakup recovery, and self-worth to deepen your understanding and build your recovery toolkit.
Remember that recognizing a trauma bond is itself an act of courage and emotional resilience. You are not broken. You are having a normal human response to an abnormal situation. With the right support, education, and patience, you can break free from this cycle and build the loving, respectful relationships you deserve. Your journey toward emotional recovery and healing and growth starts with this moment of awareness. Take the next step today by exploring your own patterns through our wellbeing assessment.
Get personalized guidance with AI coaching for emotional recovery and relationship wellness.
Start Your Healing Journey →Research Sources
This article is based on peer-reviewed research and authoritative sources. Below are the key references we consulted:
Related Glossary Articles
Frequently Asked Questions
How long does it take to break a trauma bond?
There is no fixed timeline. Breaking a trauma bond is a process that can take months to years depending on the length and intensity of the relationship, available support, and individual factors. Most therapists recommend a minimum of several months of no-contact combined with regular therapy. Progress is rarely linear, and setbacks are a normal part of recovery.
Can trauma bonding happen in friendships or family relationships?
Yes. Trauma bonding can occur in any relationship involving a power imbalance and intermittent reinforcement. Parent-child relationships, sibling dynamics, close friendships, workplace relationships, and even relationships with authority figures such as coaches or religious leaders can all involve trauma bonding. The mechanism is the same regardless of the relationship type.
Is trauma bonding the same as love?
No. While trauma bonds produce intense feelings that can mimic love, they are driven by neurochemical dependency rather than genuine mutual care and respect. Healthy love involves consistent safety, mutual respect, shared power, and the freedom to be yourself. Trauma bonds involve fear, confusion, and a loss of autonomy. Learning to distinguish between the two is a critical part of recovery.
Why do I feel withdrawal symptoms when I try to leave?
The withdrawal symptoms are real and neurobiological. The intermittent reinforcement cycle creates dopamine-driven dependency patterns similar to substance addiction. When you remove the source of those dopamine surges, your brain experiences genuine withdrawal including anxiety, depression, obsessive thoughts, and physical discomfort. These symptoms are temporary and can be managed with professional support.
Can the abuser also be trauma-bonded?
In some cases, both partners can develop aspects of trauma bonding, particularly in relationships with mutual abuse patterns. However, it is important not to use this concept to excuse abusive behavior. Regardless of their own attachment injuries, each person is responsible for their actions. A person who abuses others needs to seek their own professional help and take accountability for the harm they cause.
What type of therapy is best for trauma bonding recovery?
Several evidence-based approaches are effective. Cognitive Behavioral Therapy helps identify and restructure distorted thought patterns. EMDR (Eye Movement Desensitization and Reprocessing) processes traumatic memories. Somatic Experiencing addresses the body-based aspects of trauma. Dialectical Behavior Therapy builds emotional regulation skills. Many therapists use a combination of approaches tailored to individual needs.
How can I support someone who is trauma-bonded?
The most important thing is to remain a consistent, non-judgmental presence. Avoid ultimatums or criticism, as these can push the person closer to their abuser. Instead, express concern calmly, provide information about resources, and let them know you are available whenever they are ready. Understand that leaving is a process and they may need to attempt it multiple times before succeeding.
Take the Next Step
Ready to improve your wellbeing? Take our free assessment to get personalized recommendations based on your unique situation.
- Discover your strengths and gaps
- Get personalized quick wins
- Track your progress over time
- Evidence-based strategies